Female Incontinence – Diagnosis, Treatment and Surgery from Best Hospitals & Leading Surgeons in India.
Excellent Outcomes and Affordable Cost is assured.
Female Urinary Incontinence
Why you should choose World Class Hospitals in India for Most Advanced Treatment for Female Urinary Incontinence?



Bladder Control and Causes of Urinary Incontinence
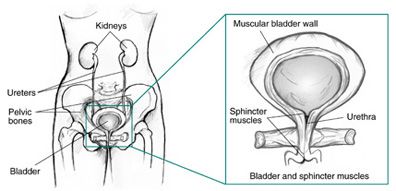
The functioning of the bladder is controlled at the local level by a micturition reflex and by the spinal cord and the brain at the higher level. The brain has centers that tell the individual if it is the right place and time to urinate. These centers are affected in conditions like Stroke, Parkinsonism, Alzheimer’s and Brain tumor because of which the person may urinate immediately after she gets the urge. The person may pass urine in bed, in a gathering etc. This is a type of urge incontinence.
At times the person may suffer from spinal cord injury. The spinal cord has nerves that carry sensation of bladder fullness from the bladder to the brain. As soon as the brain senses bladder fullness, it instructs the individual to go to the washroom to relieve him. Till such a place is found the brain sends signals through other nerves to keep the bladder opening closed. But in cases of spinal cord injury, this connection between the brain and bladder is lost as the spinal cord nerves are cut.
In this case the person gets the urgency to void urine and she does it immediately. This is also a type of urge incontinence. Also in spinal cord injury the bladder gets spastic or overactive. A little bit of urine causes reflex contraction of bladder resulting in its contraction and expulsion of small amounts of urine with increased frequency. This is known as overactive bladder.
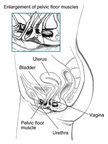
Vaginal delivery or any other surgery causes injury to the pelvic floor muscles which actually provide strength to the radial sphincter muscles that surround the opening of the bladder. As a result the bladder is never fully closed and some amount of urines leaks. This is known as genuine stress incontinence and occurs in situations where intra-abdominal pressure increases as in running, laughing, coughing, sneezing, lifting weights and obesity etc. lowered estrogen seen a few days before menses and during menopause is also responsible for incontinence as the sphincter muscles around the bladder mouth become weak.
Treatment for Female Urinary Incontinence
- Behavioral modification : Involves bladder training and timed voiding. Adjusting the time of fluid intake before bedtime or before going for a car trip or party can help avoid accidents during sleep or parties. Also timed voiding involves emptying of bladder after regular intervals. This technique is suitable for people with mechanical compression of bladder or overflow incontinence.
- Kegel Exercise : Involves strengthening of the pelvic floor muscles which help to keep the sphincter muscles tight which in turn keep the bladder outlet closed during strenuous activities. Pull in the pelvic muscles and hold for a count of 3. Then relax for a count of 3. Repeat, but do not overdo it. Work up to 3 sets of 10 repeats. This is possible with the help of biofeedback also. This helps people with stress incontinence.
- Medications : Certain medications help to relax the bladder and surrounding muscles to allow full emptying (Alpha blockers). Anticholinergics relieve the bladder muscle spasm thus preventing sudden bladder contractions.
- Neurostimulation : Of the nerves that leave the spinal cord and supply the bladder can help by modulating the nerve signals to the bladder which helps to control voiding. It is helpful in some people.
- Vaginal Devices : Like pessaries are a stiff ring that a doctor or nurse inserts into the vagina, where it presses against the wall of the vagina and the nearby urethra. The pressure helps reposition the urethra, leading to less stress leakage. If you use a pessary, you should watch for possible vaginal and urinary tract infections and see your doctor regularly.
- Surgery for Stress Incontinence :
In some women, the bladder can move out of its normal position, especially after childbirth. Different techniques have been developed by surgeons for supporting the bladder back to its normal position. The three main types of surgery are retropubic suspension and two types of sling procedures.
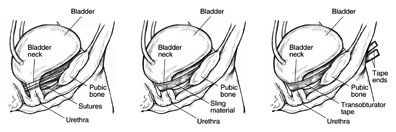
- Retropubic Suspension : Uses surgical threads called sutures to support the bladder neck. The most common retropubic suspension procedure is called the Burch procedure. In this operation, the surgeon makes an incision in the abdomen a few inches below the navel and then secures the threads to strong ligaments within the pelvis to support the urethral sphincter. This common procedure is often done at the time of an abdominal procedure such as a hysterectomy.Sling procedures are performed through a vaginal incision. The traditional sling procedure uses a strip of your own tissue called fascia to cradle the bladder neck. Some slings may consist of natural tissue or man-made material. The surgeon attaches both ends of the sling to the pubic bone or ties them in front of the abdomen just above the pubic bone.
- Midurethral Slings : are newer procedures that can be done on an outpatient basis. These procedures use synthetic mesh materials that the surgeon places midway along the urethra.
The two general types of midurethral slings areretropubic slings, such as the transvaginal tapes (TVT), andtransobturator slings (TOT). The surgeon makes small incisions behind the pubic bone or just by the sides of the vaginal opening as well as a small incision in the vagina. The surgeon uses specially designed needles to position a synthetic tape under the urethra. The surgeon pulls the ends of the tape through the incisions and adjusts them to provide the right amount of support to the urethra.
If you have pelvic prolapse, your surgeon may recommend an anti-incontinence procedure with a prolapse repair and possibly a hysterectomy.
- Catheterization : This can be done if the bladder does not empty completely in cases of poor muscle tone, past surgery, or spinal cord injury. It can be an indwelling catheter or intermittent type
We Assure Most Affordable Estimates with in 48 Hours from Top Hospitals in India.
How it Works – Get Most Affordable Treatment in India
 |
Send medical reports by WhatsApp/Email |
 |
Receive quotation(s) within 48 Hours |
 |
Get Free Medical Visa & Airport Pick up |
 |
Medical Treatment Assisted & Fly Back Home |
Frequently Asked Questions
Once you have decided that you want to get treatment in India you can email us your latest medical reports and accompanying X-Rays, MRI Scans and other relevant medical documents at help@safemedtrip.com or Call or WhatsApp us on +91-9899993637 for one to one discussion with our executives.
Once we receive your reports, we will get them reviewed by our medical experts and will send you a detailed treatment package consisting of doctor’s diagnosis, treatment plan, cost of treatment, duration of stay in hospital and duration of stay in India besides other relevant details.
Once you have confirmed to us that you want to proceed further to get treatment in India, our team will help you with the Indian medical visa assistance and documentation process. We will also help you in arranging for a comfortable local stay for you and your attendant. You don’t have to send any money in advance.
Savings can be from 30-50%, depending upon the procedure and the destination. Your treatment will be carried out from only the best hospitals in India that are NABH accredited and have specialists that are recognized globally for their expertise.
From the date you decide on one of the three affordable treatment packages offered to you. It may take 1- 3 weeks to obtain Medical Visa and book flight tickets. We have zero waiting period and you can be received at the Airport on arrival and immediately admitted at hospital and treatment will start.
Its advisable that you should not delay your treatment particularly in case of severe illnesses like Cancer, Heart or Spine etc. Early start of treatment results in quick recovery and lower expense compared to delay of treatment.
The difference in cost package due to the labour and insurance costs of the hospital operating in India, and not by the difference in the quality of treatment.
Each patient is assigned to a SafeMedTrip Patient Case Manager who will take care of every single detail ranging from arrival to send off.
Yes, of course. We will provide you with complete assistance in selecting high-quality hotels near the hospital location that fits your budget.
You will be given a complete profile of the specialist before you proceed for the treatment. On special request, we will be happy to connect you with him through a teleconferencing service facilitated by Skype.
What people say about us

Thanks for your always prompt responses to my volley of questions and concerns. I could not have managed even a step without your staff’s Excellent care. Couldn’t be happier with the Indian hospital’s Surgeon, physicians and their expertise. Very personable and professional. Would recommend to others.
All staff nurses and doctors are very attentive. Always available, kind and considerate. My stay during treatment in India was very comfortable. Will recommend for sure.
Thanks you all and God bless you
Ms. Jemila Abubakar.Refer a Patient
Get the SafeMedTrip Advantage


No Obligation – Zero Cost Assistance. We do not collect any service fee from patients. You will directly pay the hospitals after you arrive in India. We ensure Quick, Hassle Free, Affordable Treatment at World Class hospitals in India.

 Click to WhatsApp
Click to WhatsApp +91-9899993637
+91-9899993637
 The two general types of midurethral slings areretropubic slings, such as the transvaginal tapes (TVT), andtransobturator slings (TOT). The surgeon makes small incisions behind the pubic bone or just by the sides of the vaginal opening as well as a small incision in the vagina. The surgeon uses specially designed needles to position a synthetic tape under the urethra. The surgeon pulls the ends of the tape through the incisions and adjusts them to provide the right amount of support to the urethra.
The two general types of midurethral slings areretropubic slings, such as the transvaginal tapes (TVT), andtransobturator slings (TOT). The surgeon makes small incisions behind the pubic bone or just by the sides of the vaginal opening as well as a small incision in the vagina. The surgeon uses specially designed needles to position a synthetic tape under the urethra. The surgeon pulls the ends of the tape through the incisions and adjusts them to provide the right amount of support to the urethra.









